Greetings tooth fans!
This month’s blog post topic is part 2 in my series on sleep dentistry. Last time we talked about nocturnal bruxism (grinding your teeth at night), and I alluded to how sleep disordered breathing can be a contributing factor to this condition.
Today I’ll talk a little bit more about snoring and obstructive sleep apnea, and ways in which dentistry can help with these afflictions. And, hopefully, I’ll keep it interesting enough so you don’t find yourself snoring by the end of the article. 🙂
Snoring
If you’ve never slept beside (or even in the same house as) a serious snorer, consider this clip from the Simpsons (S13/E10) where Homer’s snoring is making it impossible for Marge to get any sleep at all.
How loud can snoring really be?
Think Homer’s an exaggeration? Maybe, but my Grandma used to snore so loudly, we would say she could shake the whole house. I remember sleepovers there and having the hardest time falling asleep with all that racket! I would try everything to get her to quiet down: gently tapping her arm, shaking her a little more firmly, turning on my side and pushing against her arm and side with my feet (I was four years old – consideration of others was secondary to what I thought my needs were at the time.)
The loudness of any sound is measured in decibels, or dB. According to Guinness World Records, a Swedish woman, who suffers sleep apnea, recorded peak levels of 93 decibels back in 1993. And, if it’s to be believed, The Daily Mail noted a grandmother who is said to have hit 111.6 decibels.
A study published in the Journal of Clinical Sleep Medicine classified snoring as mild at 40-50 dB, moderate at 50-60 dB, and severe at >60 dB. So an average snorer snores at approximately 50 decibels.
To put that into perspective: an electric toothbrush (55 dB), a coffee grinder (75 dB), a whistling kettle rings (an irritating 80 dB), and a jackhammer (100 dB). (thanks to Paul Virostek, a field recordist’s list here).
What causes the snoring sound?
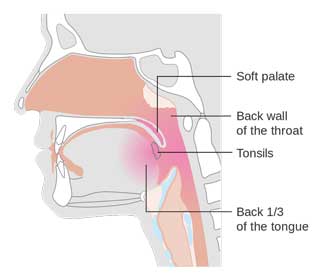
There is almost nothing worse than trying to fall asleep lying next to someone whose soft palate and oropharynx are vibrating noisily as they suck air in through their mouths in a desperate attempt to breathe.
Well I guess there is one sound worse; the sound they make when they stop!
After a while, the sound of the snoring can become rhythmic, and almost soothing, but then a sudden cessation of this sound is entirely alarming, even to a four year old. Was Grandma ok? Why wasn’t she breathing anymore? And just as soon as I would sit up to check on her, Grandma would make an even bigger, scarier noise as she suddenly caught back up with her breathing.
Today I would know that this was more than just Grandma snoring – it’s a condition called Obstructive Sleep Apnea, the treatment of which can prevent much larger health problems, but back then it was just obstructing my sleep!
Obstructive Sleep Apnea (OSA)
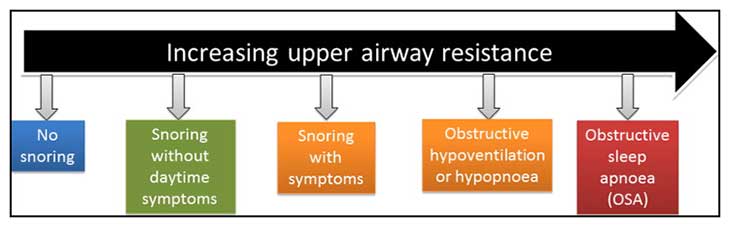
Obstructive sleep apnea is at the end of a spectrum of disturbances you can experience during the course of your sleep. The figure above illustrates that with increasing resistance in your airway, the sleep disordered breathing gets progressively worse.
What causes airway resistance?
Any structure that gets in the way of, or obstructs, your breathing. In kids it’s commonly the tonsils and the adenoids doing the obstructing, and once these are removed their breathing during sleep is significantly improved. As adults these could still be a problem, but it is less likely because these structures shrink with age.
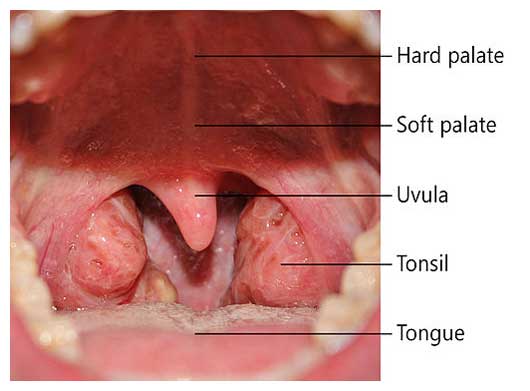
Other tissues however, lose some of their elasticity, in short they get flabby, and the uvula (the little dangly thing in your throat) and soft palate can elongate and collapse under the negative pressure when breathing, especially when we lie on our backs.
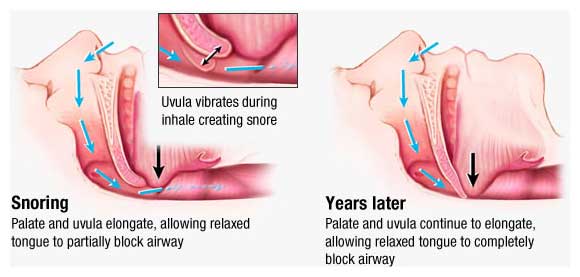
In this position, the lower jaw and the tongue drop down, placing even more pressure on the airway. This is also why rolling a snorer onto his side will often decrease or eliminate the amount of snoring. My husband snores. I am very familiar with this little trick.
What is a “sleepy” snorer?
Looking back at our spectrum of sleep disturbances, if the blockage is only slight, snoring will happen, but you’ll still be receiving enough oxygen to gain a restful night’s sleep, and thus you won’t have any symptoms during the day.
The problem really starts at the “sleepy” snorer, a person who snores all night long, and wakes up feeling unrested, potentially suffering from headaches and confusion or difficulty concentrating during the day.
That’s an indication that your body is not receiving adequate oxygen when you sleep, and it is working overtime to get the oxygen it needs.
Your sympathetic nervous system is activated causing an increase in your heart rate, an increase in your blood pressure, and an increase in bruxism.
Really, bruxism?
That’s right – your body’s “fight or flight” system is triggered because your body is fighting to get its oxygen.
Instinctively, your muscles will try to move your lower jaw forward to open the airway better. In doing so, your teeth grind together, causing wear on your teeth and straining your joints.
Sleep Hypopnea vs Sleep Apnea
Sleep hypopnea occurs when you are getting minimal air movement for longer than 10 seconds, it is marked by shallow breathing – a partial blockage. Sleep apnea is when there is no air movement. It is marked by periods of no breathing . . . you literally stop breathing.
How Do I Know if I Have OSA?
Oftentimes a patient’s spouse will make the unofficial diagnosis. It’s a scary thing when you hear a snorer stop breathing and then gasp for breath seconds later.
And sometimes we, as dentists, notice oral health signs and ask you how you’re sleeping. While it might seem like a weird question to hear at the dentist office, remember that we are your first line of defense in oral health.
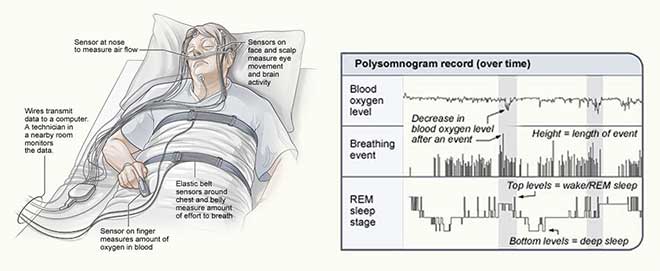
A clinical diagnosis is made using a polysomnograph, or sleep study. Both St. Mary’s and Central Maine Medical Center have sleep centers, and sometimes your doctor can give you a machine to bring home to do the sleep study in your own bed.
A sleep test registers the number of times you have an apneic or hypopneic event. These numbers are then divided by the time in the study to give you your AHI (Apnea-Hypopnea Index), which is used to make the diagnosis.
Not all loud snorers suffer from obstructive sleep apnea. However, sleep apnea is more than an annoyance to your bed partner. It’s a medical condition which places you at great risk for a variety of systemic conditions, including death.
Professional Football Hall of Fame member Reggie White and more recently, actress Carrie Fisher (Princess Leia), are two celebrities who died from complications arising from sleep apnea. The stress placed on your body from these episodes contributes to an increased risk of high blood pressure, heart attack, stroke, and diabetes.
Sleep Apnea Treatment Options & Dentistry
Depending on the severity of the condition, and the cause, a variety of treatment options are available for sleep apnea.
Improving Overall Health
Not all those who suffer from sleep apnea are overweight, but according to Jonathan Jun, M.D., a pulmonary sleep medicine sleep medicine specialist at the Johns Hopkins Center for Sleep, sleep apnea occurs in about 3% of normal weight individuals but affects over 20% of obese individuals.
“For people who are overweight or obese, weight control is very important. There are many studies showing that losing weight can either completely cure you of sleep apnea or at least make it less severe,” Jun says.
Continuous Positive Airway Pressure Therapy

The “gold standard” is the CPAP machine – a device which flows continuous positive air pressure through either a nasal or a face mask.
This has been shown to be very effective in treating all levels of sleep apnea, and is particularly necessary for severe sleep apnea. There are an assortment of CPAP masks, so don’t let some the images you see online dissuade you from seeking treatment.
Surgery
Surgery is an option in those cases where tonsils and adenoids are the culprit. This is the treatment of choice for snoring children. While adults can snore and still be ok, kids should never regularly snore (more on this on my third installment – snoring and grinding in kids). There are cases in adulthood where tonsillectomy is helpful for resolving the disordered breathing.
Additionally, in cases with an elongated uvula, a uvulopalatoplasty (usually performed with a laser), can relieve the amount of snoring as well. This tissue can sometimes grow back, however, and this procedure is not a solution for all cases.
Dental Sleep Devices

For mild to moderate cases of sleep apnea, a mandibular advancement device can be worn to move keep the lower jaw positioned forward during your sleep, thus opening the airway.
This picture may look a bit cumbersome, but it is designed to fit comfortably over both your upper and lower dentition, slightly advancing the jaw to keep the tongue forward and open the airway.
I would offer a word of caution about oral appliances: there are devices that are sold over the counter which accomplish this, but they are not as effective – or as safe – as ones constructed at a dental office. If it’s a boil and bite you make at home, it will not fit your dentition as closely as one constructed from a custom impression.
And, in any circumstance, your temporomandibular joint can be affected if an advancement device is not used appropriately, causing a TMJ disorder or orthodontic dysfunction.
We have several experienced orthodontists in the area who are far better trained to construct, monitor, and adjust these devices.

My third installment in this series will explore the consequences of grinding and snoring in kids. While this should prove to be informative and helpful for those of you with young kids at home, I’m hoping it will also go a long way towards explaining the development process that led current adults to become the sleepy snorers they are today. Stay tuned!
Love & Silent Sleeping,

Kristie Lake, DMD




